Medically Reviewed
Dr. Jose Rossello, MD, PhD, MHCM
Preventive Medicine & Public Health Specialist
Last Reviewed: April 3, 2026
Chronic diseases affect nearly 60% of American adults[1], with many people managing multiple conditions at once. Heart disease, diabetes, and cancer shape millions of lives and drive trillions of dollars in healthcare spending each year. This raises an important question about whether these widespread health problems can be stopped before they start.

Most chronic conditions are largely preventable through lifestyle changes and proactive healthcare measures. Research shows that healthy eating, regular physical activity, maintaining a healthy weight, avoiding tobacco and excessive alcohol, managing stress, and getting preventive screenings can significantly reduce the risk of developing chronic diseases. While genetics and other factors play a role, the evidence points to lifestyle modifications as powerful tools for prevention.
The reality is more complex than a simple yes or no answer. Some chronic conditions are easier to prevent than others, and factors beyond individual control like socioeconomic status, access to healthcare, and environmental conditions affect prevention outcomes. Understanding which aspects of chronic disease are truly preventable helps people make informed choices about their health.
Table of Contents
Key Takeaways
- Most chronic diseases can be prevented through lifestyle changes like healthy eating, regular exercise, and avoiding tobacco
- Individual prevention efforts must be supported by broader access to healthcare and addressing social determinants of health
- Investing in prevention reduces healthcare costs and improves quality of life for entire populations
Defining Chronic Conditions and Their Prevalence

Chronic conditions represent a major challenge to population health worldwide. Chronic diseases affect approximately 60% of Americans[2], with many people living with multiple chronic conditions that require ongoing care and management.
What Are Chronic Conditions?
Chronic diseases are conditions that last 1 year or more[3] and require ongoing medical attention or limit activities of daily living. Unlike acute illnesses that resolve quickly, these conditions persist over long periods.
The most common chronic conditions include:
- Heart disease
- Cancer
- Diabetes
- Chronic respiratory diseases (COPD and asthma)
- Stroke
- Hypertension
These conditions share similar characteristics. They develop gradually over time and often progress without proper management. Many individuals don’t experience symptoms until the disease has advanced significantly.
Global and U.S. Prevalence
The chronic disease epidemic has reached concerning levels in developed nations. In the United States, about 60% of adults live with at least one chronic condition. Many people manage more than one condition simultaneously.
Chronic conditions are the leading causes of illness, disability, and death in America[4]. The numbers continue to rise among all age groups. Younger adults show increasing prevalence of multiple chronic conditions[5], suggesting the problem extends beyond older populations.
Across OECD countries, chronic conditions such as cancer, chronic respiratory problems, and diabetes remain leading causes of death[6]. Geographic patterns also exist, with structural inequities concentrated in the southeastern region of the U.S.[7]
Leading Causes of Death and Disability
Chronic conditions dominate mortality statistics globally. Heart disease consistently ranks as the top cause of death, followed closely by cancer and stroke. These three conditions alone account for a significant portion of all deaths annually.
Beyond mortality, chronic disease creates substantial disability. Diabetes leads to complications like blindness, kidney failure, and limb amputations. COPD restricts breathing and limits physical activity. Heart disease reduces quality of life through fatigue and reduced mobility.
The economic impact is staggering. The five most costly and preventable chronic conditions cost the U.S. nearly $347 billion in 2010[8], representing 30% of total health spending. These costs continue to escalate as prevalence increases and treatment becomes more complex.
Are Chronic Conditions Preventable? The Evidence

Medical research shows that many chronic diseases can be delayed or avoided through specific actions, though the degree of preventability varies widely between conditions. The evidence reveals distinct categories of prevention, clear differences between preventable and non-preventable diseases, and important limitations based on genetics and factors beyond individual control.
Primordial, Primary, and Secondary Prevention
Public health experts classify disease prevention into three main categories. Primordial prevention stops risk factors[9] from developing in the first place by creating healthier environments and policies. Primary prevention reduces disease risk in healthy people through lifestyle changes and preventive services. Secondary prevention catches diseases early through screening and preventive care before symptoms appear.
Each level targets different stages of disease development. For example, physical inactivity, poor nutrition, tobacco use, and excessive alcohol use[10] account for more than 50% of preventable disease deaths in the United States. Addressing these factors through primary prevention can stop conditions like type 2 diabetes and heart disease before they start.
Secondary prevention includes regular screenings that detect cancer, diabetes, and cardiovascular problems early. Early detection often leads to better treatment outcomes and can prevent complications.
Preventable Versus Non-Preventable Conditions
Six in 10 American adults have chronic diseases[11], and four in 10 live with more than one condition. Not all chronic diseases fall into the preventable category.
Largely Preventable:
- Type 2 diabetes
- Heart disease
- Stroke
- Many cancers
- Chronic respiratory diseases
Limited Preventability:
- Type 1 diabetes
- Multiple sclerosis
- Rheumatoid arthritis
- Genetic disorders
The distinction matters for preventing chronic disease[8] strategies. Preventable conditions respond to lifestyle changes and environmental modifications. Non-preventable conditions may still benefit from early intervention but cannot be stopped through behavior changes alone.
Role of Genetics and Uncontrollable Factors
Genetic makeup determines some chronic disease risk regardless of lifestyle choices. A person can maintain perfect health habits yet develop conditions due to inherited genes. Age also increases disease risk in ways that cannot be controlled.
Global health[3] inequities create uncontrollable barriers to prevention. Access to healthcare, safe neighborhoods, healthy food options, and clean environments varies by income and location. These social determinants affect disease risk independent of personal choices.
Environmental exposures like air pollution and occupational hazards contribute to chronic disease development. People often cannot avoid these exposures due to where they live or work. The interaction between controllable and uncontrollable factors makes absolute prevention impossible for many individuals.
Key Modifiable Risk Factors and Their Role
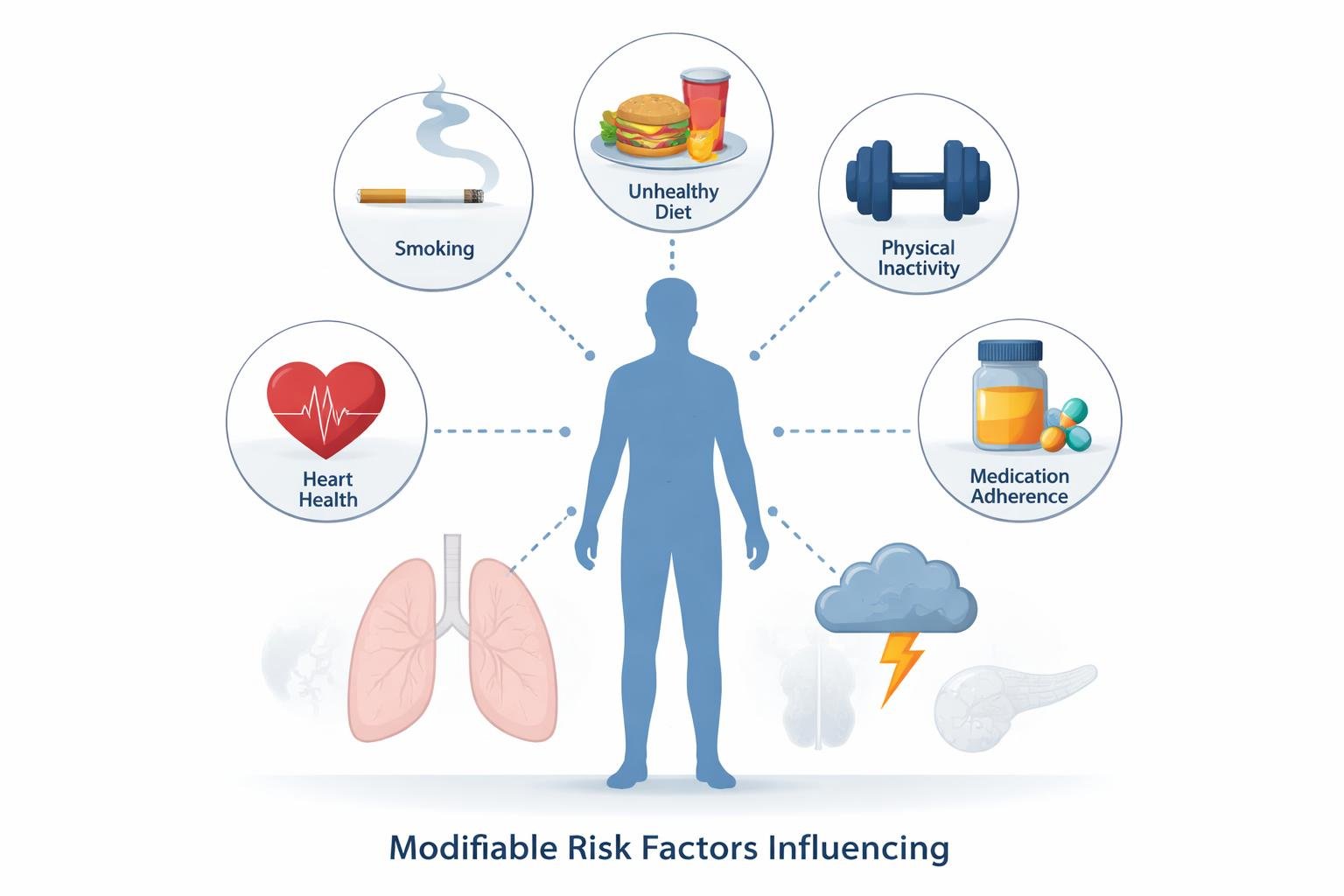
Most chronic diseases stem from a short list of behavioral risk factors[9] that people can control through lifestyle changes. Research shows that tobacco use, poor nutrition, physical inactivity, and excessive alcohol use account for the majority of preventable chronic disease cases.
Poor Nutrition and Unhealthy Diets
Poor nutrition ranks among the most significant contributors to chronic disease development. A diet lacking in fruits and vegetables while high in processed foods, saturated fats, and added sugars increases the risk of multiple conditions.
Studies found that inadequate fruit and vegetable consumption affected 84.1% of adults[12], making it the most prevalent risk factor examined. This dietary pattern contributes directly to obesity, diabetes, and heart disease.
The relationship between nutrition and body mass index is clear. People who consistently choose nutrient-poor foods tend to have higher body mass index readings. Those with severe obesity face compounded health risks that extend beyond cardiovascular problems to include joint issues, kidney disease, and cognitive decline.
A healthy diet provides the foundation for disease prevention. It includes whole grains, lean proteins, fruits, vegetables, and limited processed foods.
Physical Inactivity and Sedentarism
Physical inactivity creates substantial health risks across multiple chronic conditions. Sedentary lifestyle patterns affect a significant portion of the adult population[13] and contribute to disease development through several mechanisms.
Regular physical activity helps control weight, improves cardiovascular function, and reduces inflammation throughout the body. Without it, people experience muscle loss, decreased metabolism, and weakened immune response.
The dose-response relationship between exercise and health outcomes is well-established. Even modest increases in physical activity provide measurable benefits. People who move from completely sedentary to moderately active see the greatest relative improvements in health markers.
Modern lifestyles promote sedentarism through desk jobs, long commutes, and screen-based entertainment. Breaking up prolonged sitting periods with short movement breaks helps counter some negative effects.
Tobacco Use and Cigarette Smoking
Ever smoking contributed the most attributable risk across nine chronic conditions studied[12], alongside obesity. Cigarette smoking damages nearly every organ system and accelerates disease processes throughout the body.
Tobacco use causes direct harm to lung tissue, leading to chronic obstructive pulmonary disease and lung cancer. It also damages blood vessels, increases blood pressure, and promotes atherosclerosis. These cardiovascular effects contribute to heart disease, stroke, and kidney disease.
The impact extends beyond the respiratory and cardiovascular systems. Smoking increases inflammation markers linked to arthritis, impairs cognitive function, and worsens asthma symptoms even in those who developed the condition independent of smoking.
Former smokers show risk reduction over time, though some damage remains permanent. The earlier someone quits, the greater their potential for recovery and disease prevention.
Excessive Alcohol Use
Excessive alcohol use creates distinct health risks that differ from moderate consumption patterns. Heavy drinking damages the liver, heart, and brain while increasing cancer risk across multiple organ systems.
Alcohol affects body mass index and weight management in complex ways. It provides empty calories while impairing judgment around food choices. People who drink excessively often have poor nutrition patterns that compound their health risks.
The liver bears the primary burden of alcohol metabolism. Chronic heavy drinking leads to fatty liver disease, hepatitis, and eventually cirrhosis. These conditions progress silently until significant damage has occurred.
Alcohol also interferes with blood sugar regulation and can contribute to diabetes development. It raises blood pressure and triglyceride levels, adding to cardiovascular disease risk. Brain effects include increased risk of cognitive impairment and dementia with long-term heavy use.
Social, Environmental, and Systemic Determinants
The conditions in which people are born, grow, work, live, and age[14] shape their risk for chronic disease just as much as individual choices do. Income levels, education, neighborhood safety, and access to healthy food create powerful barriers or supports for disease prevention.
Health Disparities and Access to Care
People in different communities face vastly different health outcomes based on where they live and their access to medical services. The Mid-South region of the United States shows the highest rates of obesity, diabetes, heart disease, and cancer[15] in the country.
Health care access remains unequal across populations. People with higher incomes can afford regular checkups, preventive screenings, and early treatment. Those without insurance or living far from medical facilities often delay care until conditions become severe.
Health literacy affects how well people understand medical information and follow treatment plans. Limited health education makes it harder to recognize disease symptoms early or understand prevention strategies. These gaps in knowledge and access create health disparities that persist across generations.
Socioeconomic Status and Education
Income and education directly influence chronic disease risk through multiple pathways. Research shows that socioeconomic status affects multiple diseases through various risk factors[15], shapes health behaviors, and determines living conditions.
People with higher education levels typically:
- Understand health information better
- Make more informed medical decisions
- Have jobs with health insurance
- Live in safer neighborhoods
- Experience less chronic stress
Money provides resources to avoid health risks. Wealthier individuals can afford gym memberships, fresh produce, safer housing, and quality medical care. They also have more control over their work schedules and daily routines, which supports healthier lifestyles.
Education and income create a social gradient in health. Each step down the economic ladder corresponds with shorter life expectancy and higher rates of chronic disease.
Food Deserts and Built Environment
Food deserts are areas where residents lack access to affordable, nutritious food. These neighborhoods typically have only convenience stores and fast-food restaurants instead of grocery stores with fresh fruits and vegetables.
The built environment shapes daily physical activity levels. Communities without sidewalks, parks, or safe streets make exercise difficult. Poor lighting and high crime rates keep people indoors.
Environmental factors include:
- Air quality: Pollution increases asthma and heart disease risk
- Water safety: Contamination affects kidney health and development
- Housing conditions: Mold and lead exposure harm respiratory and neurological health
- Green space: Parks and trees reduce stress and encourage activity
These physical surroundings create different quality of life outcomes across communities. Addressing social determinants through comprehensive public health strategies[16] could reduce chronic disease burden and improve health equity.
Chronic Disease Examples: Prevention and Challenges
Different chronic conditions have varying levels of preventability based on known risk factors and available interventions. Some conditions respond well to lifestyle changes, while others prove more difficult to prevent despite best efforts.
Cardiovascular Disease and Hypertension
Cardiovascular disease remains the leading cause of death[4] in the United States. Heart disease and stroke share common risk factors that people can control through daily choices.
Blood pressure management plays a critical role in prevention. High blood pressure damages arteries over time, increasing the risk of heart attack and stroke. People can lower their blood pressure through reduced sodium intake, regular physical activity, and maintaining a healthy weight.
Key Prevention Strategies:
- Avoiding tobacco use completely
- Eating a diet low in saturated fats and sodium
- Exercising at least 150 minutes per week
- Managing stress levels
- Limiting alcohol consumption
Despite these known prevention methods, genetics and age still contribute to CVD risk. Some individuals develop heart disease even with healthy lifestyles, though their outcomes are often better than those who don’t take preventive steps.
Diabetes and Prediabetes
Type 2 diabetes develops when the body cannot properly use insulin to regulate blood sugar. Prediabetes affects millions of Americans who have elevated blood sugar levels but haven’t yet developed full diabetes.
Weight loss of just 5-10% can significantly reduce diabetes risk for people with prediabetes. Physical activity helps muscles use glucose more effectively, lowering blood sugar naturally.
Poor nutrition and physical inactivity are primary risk factors[9] for type 2 diabetes. People who consume high amounts of processed foods and sugary drinks face greater risk.
Type 2 diabetes can lead to serious complications including chronic kidney disease, vision loss, and nerve damage. CKD often develops silently over years of poorly controlled blood sugar.
Some individuals face higher genetic risk for diabetes, making prevention more challenging. However, lifestyle changes still reduce risk and delay onset even for those with family history.
Cancer and Disease Screening
Cancer includes many different diseases with varying prevention potential. Some cancers link directly to modifiable behaviors, while others have unknown or genetic causes.
Tobacco use causes approximately one-third of all cancer deaths. Lung cancer, mouth cancer, and throat cancer all have strong connections to smoking. People who quit smoking reduce their cancer risk significantly over time.
Excessive sun exposure increases skin cancer risk, which is largely preventable through sun protection and avoiding tanning beds. Regular screening helps detect skin changes early when treatment is most effective.
Preventable Cancer Risk Factors:
- Tobacco use – lung, mouth, throat cancers
- Alcohol consumption – liver, breast, colorectal cancers
- Poor diet – colorectal, stomach cancers
- HPV infection – cervical, throat cancers (vaccine available)
Disease screening saves lives by catching cancer early. Colonoscopy, mammography, and other tests detect cancer before symptoms appear. Early detection dramatically improves survival rates for many cancer types.
Alzheimer’s Disease and Dementia
Alzheimer’s disease and other forms of dementia present unique prevention challenges. Scientists don’t fully understand what causes these conditions or how to prevent them reliably.
Research suggests cardiovascular health affects brain health. High blood pressure, high cholesterol, and diabetes in midlife may increase dementia risk decades later. Managing these conditions might reduce risk, though evidence remains incomplete.
Mental stimulation, social engagement, and physical activity show some protective effects in studies. People who stay mentally and physically active throughout life may have lower dementia risk.
No proven prevention strategy exists for Alzheimer’s disease currently. Unlike heart disease or type 2 diabetes, people cannot follow clear guidelines to avoid dementia. Genetics plays a substantial role that lifestyle changes cannot override.
The lack of clear prevention methods makes dementia particularly challenging. Families and individuals face uncertainty about risk reduction strategies that actually work.
Public Health Approaches and Prevention Strategies
Public health agencies use multiple strategies to prevent and manage chronic diseases, from tracking disease patterns across populations to educating communities about risk factors. These approaches work together to catch diseases early, change unhealthy behaviors, and help people manage existing conditions more effectively.
Screening and Surveillance Programs
Public health agencies track chronic disease patterns through organized surveillance systems. The Behavioral Risk Factor Surveillance System collects data on health behaviors, chronic conditions, and preventive care use across all 50 states. This information helps identify which communities face the highest risks and where resources are needed most.
Screening programs detect diseases before symptoms appear. Regular blood pressure checks catch hypertension early, while cholesterol screenings identify cardiovascular risks. Diabetes screenings test blood sugar levels in high-risk populations. Cancer screenings like mammograms and colonoscopies find tumors at treatable stages.
These programs operate in various settings including clinics, workplaces, and community centers. Mobile health units bring screenings to underserved areas. Data from these efforts guide prevention strategies and help measure progress toward reducing chronic disease rates.
Health Promotion and Education
Health promotion programs[17] teach people how daily choices affect chronic disease risk. These initiatives target key behaviors like physical activity, nutrition, tobacco use, and alcohol consumption. Programs operate in schools, workplaces, faith-based organizations, and community settings.
Educational campaigns use multiple channels to reach different audiences. Printed materials, websites, and social media share information about disease prevention. Community health workers connect with specific populations and address cultural barriers to healthy behaviors.
Workplace wellness programs encourage employees to adopt healthier habits through fitness challenges, nutrition classes, and stress management workshops. School-based programs teach children about nutrition and physical activity early in life. These efforts aim to prevent chronic diseases before they develop.
Care Management and Disease Management Programs
Care management helps people with chronic conditions control their health and prevent complications. Disease management programs provide coordinated support for conditions like diabetes, heart disease, and asthma. Healthcare providers work with patients to create treatment plans, monitor symptoms, and adjust medications.
Chronic disease management includes regular check-ups, medication adherence support, and lifestyle counseling. Nurses and health coaches contact patients between appointments to track progress and address problems. This approach reduces emergency room visits and hospital admissions.
Telehealth expands access to care management services. Patients monitor vital signs at home and share data with their care teams remotely. Video consultations let providers adjust treatment plans without requiring office visits. These programs particularly benefit people in rural areas or those with transportation challenges.
Economic Impact and The Case for Prevention
Chronic diseases create massive financial pressure on the American healthcare system and economy. Ninety percent of the nation’s $4.9 trillion in annual health care expenditures[18] go toward treating people with chronic and mental health conditions, while lost productivity and reduced quality of life add billions more in indirect costs.
Rising Health Care Costs
The United States spends trillions on healthcare annually, with chronic diseases driving most of this spending. Nearly 60% of adults live with a chronic condition, and 40% have two or more conditions.
These patients consume a disproportionate share of resources. Just 5% of individuals with chronic diseases account for approximately 50% of total healthcare spending. This concentration reveals how expensive managing long-term conditions becomes when they progress without adequate intervention.
Roughly 194 million U.S. adults have at least one chronic condition[19], costing the economy billions of dollars each year. The financial burden extends beyond direct medical costs to include medications, hospital stays, specialist visits, and ongoing monitoring.
Productivity Losses and Societal Burden
Chronic conditions limit people’s ability to work and participate fully in daily activities. These illnesses last a year or more and restrict daily life[20] or require continuous medical attention.
Workers with chronic diseases often miss more workdays or work at reduced capacity. Some leave the workforce entirely due to disability. These productivity losses affect both individual earnings and overall economic output.
The impact extends to families and caregivers who may reduce their work hours or quit jobs to provide care. Communities face higher healthcare costs and reduced tax revenues when large portions of the population struggle with chronic illness.
Cost-Effectiveness of Preventive Measures
Proven chronic disease interventions can be cost-effective[21] because the intervention costs prove worthwhile compared to longer life and better quality of life outcomes. Prevention investments deliver returns through reduced treatment expenses and maintained productivity.
Reducing preventable deaths from major noncommunicable diseases and injuries[22] would bring substantial economic savings according to research from Harvard Chan School. Early intervention costs less than managing advanced disease stages.
Behavioral changes remain central to success. While new medications offer promise, society’s ability to reduce chronic disease costs depends heavily on lifestyle modifications like improved diet, increased physical activity, and smoking cessation.
Frequently Asked Questions
Understanding chronic diseases requires examining the specific behaviors that influence risk, the medical and financial challenges they create, and how early action can change health outcomes. These conditions affect nearly 60% of American adults and stem from identifiable causes that individuals can address.
What lifestyle modifications can reduce the risk of developing chronic diseases?
Four main risk factors[9] account for most preventable chronic diseases: tobacco use, poor nutrition, physical inactivity, and excessive drinking. People who avoid these behaviors significantly lower their chances of developing serious health problems.
Regular exercise plays a critical role in prevention. Adults should aim for at least 150 minutes of moderate activity like brisk walking each week, plus muscle-strengthening exercises twice weekly.
A balanced diet includes fruits, vegetables, whole grains, lean protein, and low-fat dairy while limiting added sugars, saturated fats, and sodium. Getting at least 7 hours of sleep daily also helps prevent diabetes, heart disease, obesity, and depression.
Quitting smoking reduces the risk of heart disease, cancer, type 2 diabetes, and lung disease, even for people who have smoked for many years. Drinking fluoridated water, brushing with fluoride toothpaste twice daily, and flossing help prevent oral diseases that affect millions of Americans.
What are the most effective strategies for the management of chronic illness?
Regular preventive care allows doctors to catch chronic diseases early when they are easier to manage. Patients should visit their doctor and dentist regularly for screenings and checkups.
Following prescribed treatment plans consistently helps control symptoms and slow disease progression. This includes taking medications as directed, attending follow-up appointments, and monitoring vital signs or blood sugar levels at home when recommended.
Maintaining healthy lifestyle habits remains important even after diagnosis. The same behaviors that prevent chronic diseases also help manage existing conditions and prevent complications.
Patients with a family history of chronic disease should share this information with their doctor. Healthcare providers can then recommend specific screening schedules and prevention strategies tailored to individual risk factors.
How do symptoms vary among different chronic diseases?
The four main types of chronic diseases[23] are cardiovascular diseases like heart attacks and stroke, cancers, chronic respiratory diseases such as asthma, and diabetes. Each category presents distinct symptoms and health challenges.
Cardiovascular diseases may cause chest pain, shortness of breath, or weakness in the limbs. Diabetes often leads to increased thirst, frequent urination, and fatigue.
Chronic respiratory diseases typically involve breathing difficulties, wheezing, and persistent coughing. Cancer symptoms vary widely depending on the type and location but may include unexplained weight loss, pain, or unusual lumps.
Many chronic diseases develop slowly and show few symptoms in early stages. This makes regular screening essential for early detection.
What is the economic burden associated with chronic diseases for individuals?
Just 5% of individuals with chronic diseases[1] account for approximately 50% of healthcare spending. These conditions create substantial financial strain on patients and families.
People with chronic diseases face ongoing costs for medications, doctor visits, medical equipment, and treatments. Many require regular monitoring and specialized care that adds up over time.
About 40% of adults have two or more chronic conditions, which compounds both health challenges and medical expenses. Lost work time and reduced earning capacity further increase the economic impact on individuals and households.
Insurance may not cover all treatment costs, leaving patients responsible for copayments, deductibles, and uncovered services. Preventive measures cost significantly less than managing chronic diseases long-term.
What are the primary causes of chronic diseases?
Physical inactivity, poor nutrition, tobacco use, and excessive alcohol use[10] are the leading risk factors for preventable chronic disease. These four factors account for more than 50% of preventable disease deaths in the United States.
These behaviors contribute to cancer, chronic respiratory diseases, type 2 diabetes, and cardiovascular disease. Lifestyle choices related to diet, smoking, physical activity, and alcohol deeply affect disease development.
Genetics and family history also play a role in chronic disease risk. People with relatives who had heart disease, diabetes, cancer, or osteoporosis face higher chances of developing these conditions themselves.
Environmental factors, age, and access to healthcare influence chronic disease rates. However, modifying controllable risk factors remains the most effective way to reduce individual risk.
In what ways can early detection and intervention influence the progression of chronic conditions?
Preventive health care aims to block or delay the development of illness[24] and limit the negative impacts of chronic diseases. Addressing health concerns early improves long-term health outcomes.
Screenings detect diseases before symptoms appear, when treatment is often simpler and more effective. Cancer screening tests, diabetes testing, and cardiovascular assessments identify problems at manageable stages.
Early intervention allows patients to make lifestyle changes and begin treatment before conditions worsen. This can slow or even reverse disease progression in some cases.
Regular checkups help doctors monitor risk factors like high blood pressure or elevated blood sugar before they develop into serious conditions. Catching prediabetes, for example, gives people the opportunity to prevent full diabetes through diet and exercise changes.
Post Views: 4
References
- Just a moment…. https://www.amjmed.com/article/S0002-9343%2825%2900195-0/fulltext Accessed April 4, 2026
- The Growing Burden of Chronic Diseases. https://nihcm.org/publications/the-growing-burden-of-chronic-diseases Accessed April 4, 2026
- 403. https://pmc.ncbi.nlm.nih.gov/articles/PMC8051856/ Accessed April 4, 2026
- About Chronic Diseases | Chronic Disease. https://www.cdc.gov/chronic-disease/about/index.html Accessed April 4, 2026
- Trends in Multiple Chronic Conditions Among US Adults, By Life Stage, Behavioral Risk Factor Surveillance System, 2013–2023. https://www.cdc.gov/pcd/issues/2025/24_0539.htm Accessed April 4, 2026
- Just a moment…. https://www.oecd.org/en/topics/chronic-diseases.html Accessed April 4, 2026
- Chronic Disease Prevalence in the US: Sociodemographic and Geographic Variations by Zip Code Tabulation Area. https://www.cdc.gov/pcd/issues/2024/23_0267.htm Accessed April 4, 2026
- 403. https://pmc.ncbi.nlm.nih.gov/articles/PMC8352511/ Accessed April 4, 2026
- Preventing Chronic Diseases: What You Can Do Now | Chronic Disease. https://www.cdc.gov/chronic-disease/prevention/index.html Accessed April 4, 2026
- 403. https://pmc.ncbi.nlm.nih.gov/articles/PMC10830426/ Accessed April 4, 2026
- Chronic Disease Key Facts. https://nam.edu/product/health-basics-chronic-disease/ Accessed April 4, 2026
- ScienceDirect. https://www.sciencedirect.com/science/article/pii/S0091743519300179 Accessed April 4, 2026
- 403. https://pmc.ncbi.nlm.nih.gov/articles/PMC11675894/ Accessed April 4, 2026
- Social determinants of health. https://www.who.int/health-topics/social-determinants-of-health Accessed April 4, 2026
- 403. https://pmc.ncbi.nlm.nih.gov/articles/PMC5328595/ Accessed April 4, 2026
- ResearchGate. https://www.researchgate.net/publication/385971630_Understanding_the_Role_of_Social_Determinants_in_Shaping_Chronic_Disease_Outcomes_A_Comprehensive_Review Accessed April 4, 2026
- Chronic Disease Prevention. https://www.phi.org/our-work/focus-areas/chronic-disease-prevention/ Accessed April 4, 2026
- Fast Facts: Health and Economic Costs of Chronic Conditions | Chronic Disease. https://www.cdc.gov/chronic-disease/data-research/facts-stats/index.html Accessed April 4, 2026
- The Cost of Chronic Disease: An Economist’s Perspective on Making America Healthy Again – September 2, 2025. https://schaeffer.usc.edu/research/the-cost-of-chronic-disease-an-economists-perspective-on-making-america-healthy-again/ Accessed April 4, 2026
- These illnesses last a year or more and restrict daily life. https://www.jec.senate.gov/public/_cache/files/05d4343b-91e3-4c0f-bd50-9376fa86a2ce/jec-chronic-conditions-final.pdf Accessed April 4, 2026
- Health and Economic Benefits of Chronic Disease Interventions | National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP). https://www.cdc.gov/nccdphp/priorities/index.html Accessed April 4, 2026
- Economic savings ‘substantial’ from reducing avoidable deaths from chronic disease and injury. https://hsph.harvard.edu/news/economic-savings-substantial-from-reducing-avoidable-deaths-from-chronic-disease-and-injury/ Accessed April 4, 2026
- Noncommunicable diseases. https://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases Accessed April 4, 2026
- Preventive Care. https://www.cms.gov/priorities/innovation/key-concepts/preventive-care Accessed April 4, 2026