Medically Reviewed
Dr. Jose Rossello, MD, PhD, MHCM
Preventive Medicine & Public Health Specialist
Last Reviewed: April 27, 2026
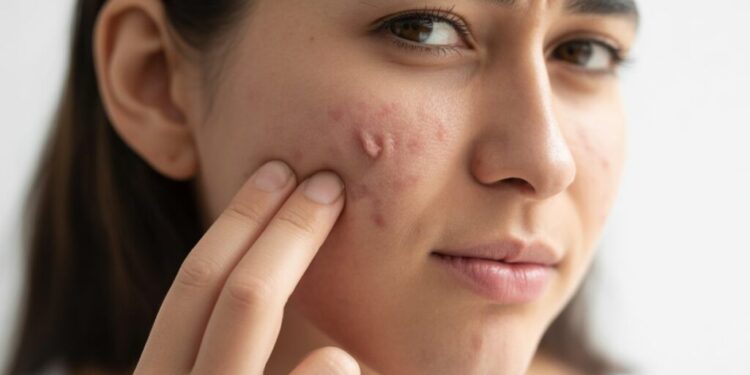
You wash your face twice daily, avoid touching your skin, and follow every skincare tip you find online. Yet pimples keep appearing without warning. Many people struggle with persistent breakouts well into their 20s, 30s, and beyond, leaving them frustrated and confused about what they’re doing wrong.

Adult acne affects up to 88% of people at some point, and the causes often have nothing to do with poor hygiene or your basic skincare habits. The truth is that breakouts stem from a complex mix of factors working beneath your skin’s surface. Everything from hormone fluctuations to modern stress[1] can trigger oil glands and clog pores, even if you sailed through your teenage years with clear skin.
Understanding why breakouts happen and what specific triggers affect your skin makes all the difference in finding real solutions. From the biological process behind clogged pores to hidden culprits like phone screens and pillowcases, the path to clearer skin starts with identifying what’s actually causing your problems.
Table of Contents
Key Takeaways
- Acne forms when dead skin cells, oil, and bacteria combine to clog pores and cause inflammation
- Common triggers include hormones, stress, certain skincare products, diet, and everyday items that touch your face
- Effective treatment requires consistent routines with the right ingredients, and professional help may be needed[2] if breakouts persist after eight weeks
How Acne Forms: The Biological Process
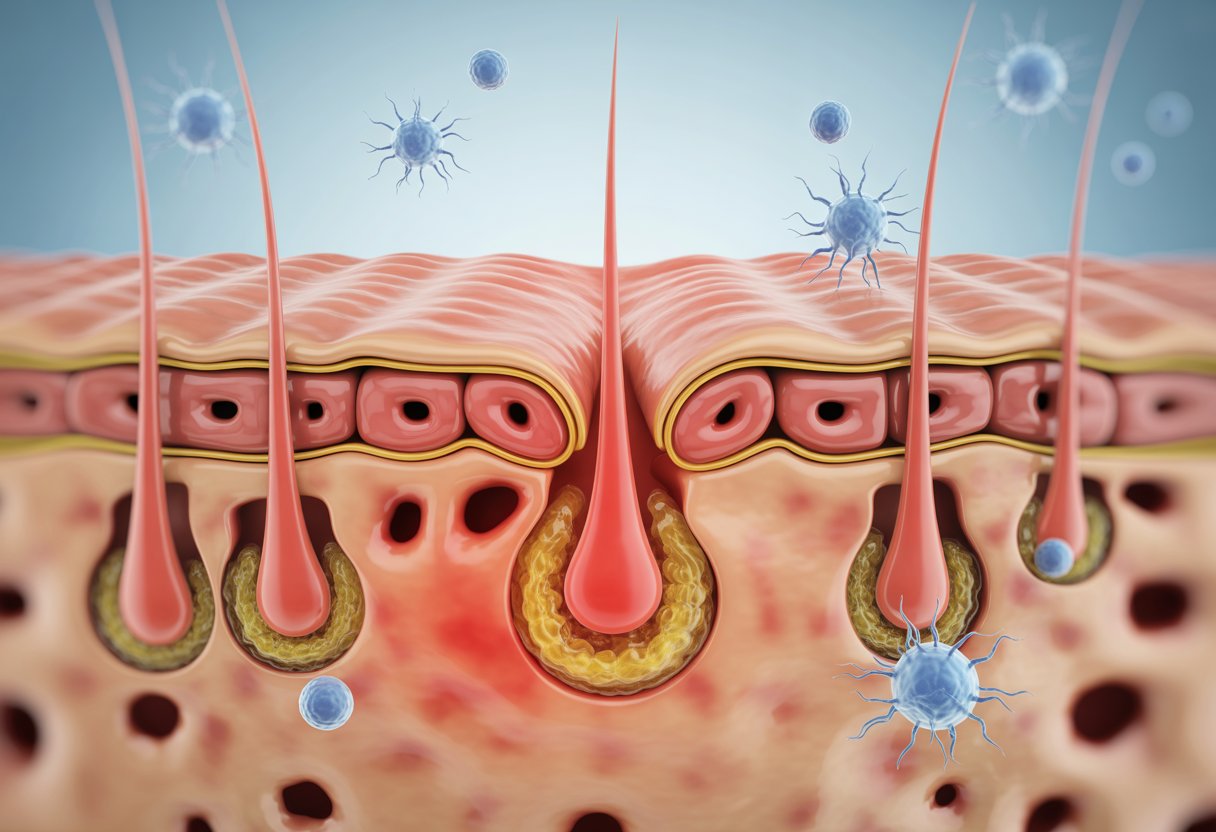
Acne vulgaris develops through a complex chain of events involving oil production and inflammation. The process starts deep within the skin’s sebaceous glands and progresses through multiple stages before visible pimples appear.
The Role of Sebaceous Glands and Sebum Production
Sebaceous glands sit beneath the skin’s surface and produce sebum, an oily substance that normally protects and moisturizes the skin. These glands connect to hair follicles, creating small channels where sebum travels to reach the skin’s surface.
When hormone levels change, sebaceous glands can produce excess sebum. This overproduction creates an environment where problems begin to develop. The sebum’s composition can also shift, becoming thicker and stickier than normal.
Certain factors trigger the glands to work overtime. Androgens, hormones present in both males and females, stimulate these glands to enlarge and produce more oil. The glands respond by pumping out higher volumes of sebum, which sets the stage for acne development.
The Cycle of Clogged Pores and Inflammatory Responses
Inflammation appears in the skin right from the start[3] of acne formation, not just at the end. This early inflammation triggers skin cells to overproduce keratin, a sticky protein that lines the pores.
The combination of excess sebum and keratin creates clogged pores, also called comedones. When these clogs remain under the skin, they form whiteheads. When they reach the surface and oxidize, they turn into blackheads.
Trapped sebum inside clogged pores creates a breeding ground for bacteria. The buildup increases pressure on the pore walls. Eventually, this pressure causes the pore to rupture, releasing its contents into surrounding skin tissue.
The body treats this rupture as a foreign invasion. Immune cells flood the area, creating the red, swollen bumps known as inflammatory acne. This response leads to pustules and other visible pimples on the skin’s surface.
Understanding Different Types of Acne
Not all breakouts are the same, and identifying the specific type of acne someone has is essential for choosing the right treatment approach. Some blemishes form from clogged pores while others develop from deeper inflammation beneath the skin’s surface.
Whiteheads, Blackheads, and Pimples
Whiteheads appear as small, flesh-colored bumps that form when dead skin cells and oil trap bacteria inside a closed pore. The pore remains covered by skin, which gives these blemishes their characteristic white or pale appearance.
Blackheads develop when pores become clogged but remain open at the surface. The dark color isn’t dirt but rather oxidized melanin and sebum exposed to air. Both blackheads and whiteheads[4] fall under comedonal acne, which is generally easier to treat than inflammatory types.
Pimples occur when bacteria, oil, and dead skin cells cause inflammation in the pore. These raised, red bumps often contain pus and can be tender to the touch. Related conditions like folliculitis involve inflammation of hair follicles, while acne mechanica results from friction and pressure on the skin from sports equipment or tight clothing. Acne cosmetica develops when certain makeup or skincare products clog pores.
Cystic and Inflammatory Acne Variants
Cystic acne represents one of the most severe forms of breakouts. These painful, deep lumps form beneath the skin’s surface when pores become blocked and infected deep within the skin tissue. Unlike surface pimples, cysts feel like soft, fluid-filled bumps and carry a higher risk of leaving acne scars.
Inflammatory acne[5] includes papules, pustules, nodules, and cysts that all involve swelling and redness. Papules are small, raised bumps without visible pus, while pustules contain yellow or white pus at their center. Nodules are large, hard bumps deep under the skin that can persist for weeks or months.
Acne keloidalis nuchae is a specific inflammatory condition that primarily affects the back of the neck and scalp. It causes raised, thick scars that can become permanent without proper treatment. This variant requires specialized care from a dermatologist.
Common Daily Triggers and Hidden Causes
Many breakouts stem from everyday habits that transfer bacteria and oil to the skin. Simple changes to daily routines can prevent breakouts and reduce acne flare-ups significantly.
Touching Your Face and Everyday Objects
People touch their faces hundreds of times each day without realizing it. Every touch transfers dirt, oil, and bacteria from hands directly onto the skin. This creates the perfect environment for clogged pores and new pimples.
Cell phones are major culprits. They collect bacteria throughout the day and press against the face during calls, trapping heat and sweat. This can lead to breakouts along the cheek and jawline where the phone makes contact.
Common objects that cause breakouts:
- Cell phones
- Computer keyboards
- Door handles
- Gym equipment
To avoid touching your face, people can start by becoming more aware of the habit. Washing hands frequently helps reduce the bacteria transferred during accidental touches. Cleaning phones with alcohol wipes daily removes built-up bacteria and oils.
Unwashed Pillowcases and Dirty Makeup Brushes
Pillowcases collect dead skin cells, oil, hair products, and bacteria every night. Sleeping on the same pillowcase for weeks means pressing the face into accumulated grime for eight hours straight.
Clean makeup brushes are equally important. Brushes should be washed once a week[6] to remove trapped bacteria and old makeup. Dirty brushes spread bacteria across the face with every use and can damage the skin barrier.
Cleaning schedule:
- Pillowcases: Every 2-3 days
- Makeup brushes: Weekly
- Face towels: After each use
Using a fresh pillowcase more often gives the skin a cleaner surface each night. People who can’t wash pillowcases frequently can flip them to the clean side after one night.
Sweat, Friction, and Tight Clothing
Acne mechanica develops when heat and sweat get trapped against the skin[6] with constant rubbing. Athletes often experience this type of acne under helmets, straps, and tight workout gear.
Face masks can cause breakouts called mascne. The combination of trapped moisture, friction, and restricted airflow creates an ideal environment for bacteria growth.
Items that cause friction acne:
- Sports helmets and headbands
- Bra straps and underwire
- Tight collars and turtlenecks
- Backpack straps
Showering immediately after sweaty activities removes bacteria before it clogs pores. Wearing moisture-wicking fabrics helps keep skin drier during exercise. People should choose looser-fitting clothes when possible and wash workout gear after each use. Those experiencing bumps on the back of the neck from helmets or frequent shaving should see a dermatologist, as this could indicate acne keloidalis nuchae rather than standard breakouts.
Hormonal Influences and Fluctuations

Hormones act as chemical messengers that control oil production and skin cell activity. When these hormones shift during puberty, monthly cycles, or adulthood, they can trigger breakouts even in people who never had acne before.
Puberty, Menstruation, and Androgens
Androgens like testosterone surge during puberty and signal oil glands to produce excess sebum. This spike in sebum production clogs pores and creates an ideal environment for acne-causing bacteria. Both males and females produce androgens, though males typically have higher levels.
During the menstrual cycle, hormonal fluctuations throughout the month directly impact skin behavior[7]. Estrogen rises during the first half of the cycle, often leading to clearer skin. After ovulation, progesterone increases and causes pores to swell and retain fluid.
This luteal phase often brings more breakouts in the week before menstruation starts. The skin becomes oilier and more prone to clogged pores. Many women notice these predictable patterns of acne flare-ups that align with their monthly cycle.
Adult and Hormonal Acne Patterns
Hormonal acne can affect adults[8] long after teenage years end. This type typically appears along the jawline, chin, and lower cheeks rather than the forehead. Adult acne responds differently to treatment than teenage acne because the underlying cause involves hormone imbalances rather than just excess oil.
Women often experience adult acne during pregnancy, perimenopause, or menopause when estrogen levels drop. As estrogen declines, the balance shifts toward androgens, which increases oil production even in dry or mature skin.
Conditions like polycystic ovary syndrome (PCOS) cause elevated androgen levels that lead to persistent breakouts. Stress also triggers hormonal changes by raising cortisol levels, which can worsen existing acne or trigger new breakouts. These patterns require addressing the hormonal root cause rather than just treating surface symptoms.
Skincare Products and Regimen Mistakes

Your products might be working against you instead of helping your skin clear up. Common mistakes include using ingredients that clog pores, scrubbing too hard, or skipping important steps in your daily routine.
Comedogenic Ingredients in Skincare and Makeup
Many popular skincare and makeup products contain comedogenic ingredients that block pores and trigger breakouts. These pore-clogging substances sit on the skin’s surface and trap oil, dead skin cells, and bacteria inside follicles.
Common comedogenic ingredients include coconut oil, cocoa butter, and certain silicones found in primers and foundations. Even products labeled as “natural” or “organic” can contain these problematic ingredients. People who continue breaking out despite having a good skincare routine[9] may be unknowingly using comedogenic products.
The solution involves switching to non-comedogenic products that won’t clog pores. Look for labels that specifically state “non-comedogenic” on cleansers, moisturizers, and makeup. A non-comedogenic moisturizer helps hydrate skin without causing new blemishes.
Makeup tools also play a role in breakouts. Dirty brushes and sponges collect oil, dead skin, and bacteria that transfer back onto the face. Clean makeup brushes at least once a week with gentle soap and warm water to prevent product buildup from causing acne.
Over-Exfoliating and Harsh Cleansers
Scrubbing the face too often or using harsh products damages the skin barrier and makes acne worse. Over-exfoliating strips away protective oils and causes irritation, redness, and increased breakouts.
Many people believe that stronger cleansers work better for oily or acne-prone skin. Foaming cleansers with sulfates can feel satisfying but often remove too much natural oil. This triggers the skin to produce even more sebum to compensate, creating a cycle of excess oil and breakouts.
The skin needs time to repair itself between exfoliation sessions. Using chemical exfoliants like salicylic acid or physical scrubs more than 2-3 times per week can lead to a compromised skin barrier. When the barrier weakens, skin becomes more sensitive to bacteria and environmental irritants.
A gentle cleanser works better for most skin types, including acne-prone skin. These formulas clean effectively without stripping or irritating. People should wash their face twice daily with lukewarm water and pat skin dry rather than rubbing with a towel.
Missed Steps in a Consistent Skincare Routine
Skipping products or applying them incorrectly reduces their effectiveness at preventing breakouts. A complete skincare routine requires following the same steps morning and night without exception.
One common mistake involves using acne treatments as spot treatments only. Applying products only to existing pimples[9] does nothing to prevent new breakouts from forming. Active ingredients work best when applied to all acne-prone areas in a thin, even layer.
Another issue occurs when people don’t wait long enough to see results. Most acne treatments take 6-8 weeks of consistent use before showing improvement. Some people experience skin purging during the first few weeks, where breakouts temporarily increase as the skin adjusts to new ingredients. This phase passes with continued use.
Moisturizer often gets skipped by people with oily skin who fear it will make breakouts worse. However, all skin types need hydration to maintain a healthy barrier. Without moisturizer, skin can become dehydrated and produce more oil to compensate.
Diet, Lifestyle, and Environmental Factors

What you eat, how you sleep, and where you spend your time all affect your skin. Foods like sugar and dairy can trigger inflammation[10], while poor sleep and stress change hormone levels that worsen breakouts.
High Glycemic Foods and Sugar Intake
High glycemic foods raise blood sugar quickly and directly impact skin health. When blood sugar spikes, the body produces more insulin, which triggers oil glands to make excess sebum. This extra oil clogs pores and creates an ideal environment for acne-causing bacteria.
Sugar accelerates skin aging[11] by breaking down collagen into advanced glycation end products. These compounds reduce skin elasticity and contribute to inflammation throughout the body, including the skin.
Common high glycemic foods that may worsen acne[6] include:
- White bread and refined grains
- Sugary breakfast cereals
- Candy and desserts
- Sodas and sweetened drinks
- Fast food
People with acne-prone skin should focus on low glycemic alternatives like whole grains, vegetables, and fruits. These foods help maintain steady blood sugar levels and reduce inflammation.
Dairy, Smoking, and Pollution
Milk and other dairy products contain hormones that can stimulate oil production in the skin. Research shows a strong connection between dairy consumption and acne breakouts, particularly in adults.
Cigarette smoking changes the composition of natural oils[6] on the face. Smokers often develop large, cyst-like pimples scattered across their face. This type of adult acne is especially common in women who smoke.
Air pollution exposes skin to harmful particles that settle on the surface and penetrate pores. These pollutants trigger inflammation and oxidative stress. Travelers may notice breakouts after exposure to unfamiliar pollution levels in new cities.
People can protect their skin by limiting dairy intake, avoiding cigarettes, and cleansing their face thoroughly after spending time in polluted environments.
Stress and Sleep Deprivation
Stress increases cortisol production, a hormone that weakens the immune system and promotes inflammation. High cortisol levels make existing acne worse and trigger new breakouts, particularly along the jawline.
Poor sleep habits contribute to skin inflammation in multiple ways. Insufficient sleep links to many inflammatory diseases[6], and studies show a two-way relationship between poor sleep and acne. People who sleep poorly are more likely to have breakouts, and those with acne often struggle to sleep well.
Sleep deprivation also disrupts hormone balance and impairs the skin’s ability to repair itself overnight. The body needs adequate rest to maintain healthy skin function and prevent breakouts.
Managing stress through regular exercise, meditation, or other relaxation techniques helps control cortisol levels. Getting seven to nine hours of quality sleep each night gives skin time to heal and regenerate properly.
The Impact of Haircare and Body Products
Your skincare routine might be flawless, but the products you use on your hair and body can still trigger breakouts. Ingredients in shampoos, conditioners, and styling products often migrate to your face, while clothing and certain body products create conditions for acne to develop.
Pomade Acne and Acne Cosmetica
Pomade acne develops when hair products containing oils, waxes, or silicones transfer onto the skin. This condition typically appears along the hairline, forehead, temples, and back of the neck where hair makes contact with skin.
Hair care products can cause whiteheads and other types of acne[12] in these areas. The heavy ingredients in styling products, leave-in conditioners, and hair oils create a film on the skin that blocks pores.
Acne cosmetica refers to breakouts caused by any cosmetic product, including haircare items. Common triggers include:
- Sulfates in shampoos that irritate skin
- Coconut oil and shea butter in conditioners
- Silicones in anti-frizz serums
- Heavy styling waxes and pomades
People who sleep with wet hair or let conditioner run down their face in the shower face higher risk. Switching to non-comedogenic hair products and keeping hair off the face can prevent these breakouts.
Body Acne and Clothing Choices
Body acne develops on the back, chest, and shoulders when sweat, bacteria, and friction combine. Tight clothing traps heat and moisture against the skin, creating an environment where acne-causing bacteria thrive.
Acne mechanica occurs when repeated friction from clothing, backpacks, or sports equipment rubs against skin. Athletes often experience this type of breakout from helmets, shoulder pads, or tight workout gear.
Clothing-related triggers include:
- Synthetic fabrics that don’t breathe
- Tight sports bras and athletic wear
- Backpack straps rubbing shoulders
- Dirty workout clothes worn multiple times
Folliculitis can develop when hair follicles become inflamed from friction and sweat. This appears as small red bumps that resemble acne but involve infected hair follicles rather than clogged pores[6].
Wearing loose, breathable cotton clothing and showering immediately after sweating helps prevent body breakouts. Washing workout clothes after each use removes bacteria and oils that contribute to acne.
Treatment Resistance and Skin Purging

New acne products can cause temporary worsening that looks like treatment failure, while genuinely ineffective treatments require a different approach. Skin purging occurs when active ingredients increase cell turnover[13], bringing existing congestion to the surface faster than normal.
Recognizing the Signs of Skin Purging
Skin purging appears in areas where breakouts typically occur, such as the chin and forehead. It presents as small pustules, blackheads, or whiteheads accompanied by dry, flaky skin and mild tenderness.
Purging happens shortly after introducing a new skincare product[14], usually within the first few days of use. The most common triggers include retinol, retinoic acid, glycolic acid, lactic acid, and salicylic acid. Prescription acne treatments like isotretinoin can also cause purging.
The timeline helps distinguish purging from new breakouts. Purging should subside within four to six weeks as the skin adjusts to increased cell turnover. Spots that appear in unusual locations or continue beyond six weeks likely indicate new acne rather than purging.
People with sensitive, dry, or eczema-prone skin experience more frequent acne flare-ups during the purging phase. The skin may develop a pink tinge and feel more tender than typical breakouts.
When Acne Treatments Stop Working
Treatment resistance develops when acne stops responding to previously effective products or prescription-strength acne medications. Unlike purging, which improves within weeks, resistant acne persists or worsens despite continued treatment.
Bacteria adaptation represents a common cause of prescription acne treatments losing effectiveness. Overuse of the same active ingredient allows acne-causing bacteria to develop resistance over time.
Treatment fatigue can also reduce efficacy. The skin becomes less responsive to familiar ingredients, requiring either higher concentrations or different prescription-strength acne formulations. Hormonal changes, stress, and dietary shifts may diminish treatment results even when the medication remains effective for others.
Effective Over-the-Counter and Prescription Solutions

Treatment options range from drugstore products containing proven active ingredients to powerful prescription medications that target severe breakouts. The right approach depends on the type and severity of acne someone experiences.
Benzoyl Peroxide and Salicylic Acid
Benzoyl peroxide kills acne-causing bacteria and helps unclog pores. It’s available in concentrations from 2.5% to 10%, though lower strengths often work just as well with less irritation. This ingredient can bleach fabrics, so users should apply it carefully and let it dry completely.
Salicylic acid is a BHA that dissolves the debris inside pores. It works best for blackheads and whiteheads because it can penetrate oil. Most over-the-counter products contain 0.5% to 2% salicylic acid.
Key differences between these ingredients:
| Ingredient | How It Works | Best For |
|---|---|---|
| Benzoyl Peroxide | Kills bacteria, reduces inflammation | Inflamed pimples, cystic acne |
| Salicylic Acid | Exfoliates inside pores | Blackheads, whiteheads, oily skin |
People with sensitive skin should start with lower concentrations and gradually increase if needed. Finding products labeled non-acnegenic and oil-free[15] helps prevent additional breakouts while treating existing acne.
Topical Retinoids and Prescription Options
Retinoids speed up cell turnover and prevent clogged pores. Adapalene is available over-the-counter at 0.1% strength and works well for mild to moderate acne. Prescription-strength retinoids like tretinoin offer higher concentrations for stubborn cases.
Tretinoin requires a prescription and comes in various strengths. It treats acne while improving skin texture and reducing dark spots from old breakouts. Users typically see results after 8 to 12 weeks of consistent use.
For severe acne that doesn’t respond to topical treatments, dermatologists may prescribe isotretinoin. This oral medication dramatically reduces oil production and provides long-term clearing for many patients. It requires close medical supervision due to potential side effects.
Online services like Curology offer personalized prescription formulas that combine multiple active ingredients. These custom treatments can include retinoids, antibiotics, and other prescription-strength acne fighters tailored to individual skin needs.
Choosing the Right Spot Treatments
Spot treatments deliver concentrated ingredients directly to active breakouts. Products containing 5% to 10% benzoyl peroxide work quickly on inflamed pimples by reducing bacteria and swelling.
Salicylic acid spot treatments help dry out blemishes without excessive peeling. Some formulas combine multiple ingredients like sulfur or tea tree oil for added benefits. The key is applying these products only to affected areas, not the entire face.
Application tips for spot treatments:
- Apply to clean, dry skin
- Use a thin layer only on the pimple
- Avoid layering multiple spot treatments at once
- Apply before moisturizer but after any other acne treatments
AHAs like glycolic acid can help fade the red or dark marks left behind after breakouts heal. These shouldn’t replace traditional acne treatments but can complement them. People using multiple active ingredients should introduce them slowly to avoid irritation and monitor how their skin responds.
Building a Sustainable, Preventive Skincare Routine
A consistent approach to skin care helps prevent breakouts before they start. The right products and daily habits work together to keep skin clear without causing irritation or clogged pores.
Washing and Moisturizing the Right Way
People with acne-prone skin need to wash their face twice daily with a gentle cleanser. Harsh soaps strip natural oils and trigger the skin to produce more oil, which leads to more breakouts.
A good gentle cleanser removes dirt and excess oil without leaving skin tight or dry. The best time to wash is in the morning and before bed. Lukewarm water works better than hot water, which can irritate the skin.
After cleansing, applying a non-comedogenic moisturizer keeps skin balanced. Many people skip this step because they think moisturizer will make their skin oily. This is wrong. When skin gets too dry, it makes more oil to compensate.
Look for moisturizers with hyaluronic acid, which hydrates without clogging pores. A non-comedogenic moisturizer won’t block pores or cause new breakouts. Apply it while skin is still slightly damp to lock in moisture.
The Importance of Non-Comedogenic Sunscreen
Sunscreen protects skin from damage that can worsen acne and cause dark spots. Many people avoid sunscreen because they think it will cause breakouts. The key is choosing the right formula.
Non-comedogenic sunscreen is made to not clog pores. It should be part of every morning skincare routine, even on cloudy days. UV rays can make acne scars darker and more visible over time.
Mineral sunscreens with zinc oxide or titanium dioxide work well for sensitive, acne-prone skin. Chemical sunscreens are also fine if they’re labeled non-comedogenic. Apply sunscreen as the last step after moisturizer.
Long-Term Habits for Acne-Prone Skin
Building sustainable skincare habits[16] means sticking to the same routine every day. Switching products too often doesn’t give skin time to adjust and improve.
Clean pillowcases weekly and avoid touching the face throughout the day. Phones, hands, and hair carry oils and bacteria that transfer to skin. These small actions add up over time.
Keep track of what products work and which ones cause problems. Most skincare products need 4-6 weeks to show results. Patience matters more than buying new products every few weeks.
Key habits to maintain:
- Wash face twice daily
- Use products in the same order each time
- Replace makeup sponges and brushes regularly
- Remove makeup before bed every night
- Stay hydrated and get enough sleep
Frequently Asked Questions
Breakouts can appear suddenly due to hormone shifts, new products, or stress triggers. The location and type of bumps often point to specific causes that require different approaches.
What causes a sudden breakout of pimples on the face?
Sudden breakouts usually happen when something triggers the oil glands to produce more sebum or when dead skin cells block pores. Common culprits include hormone fluctuations, stress, new skincare products, or medications[1].
Stress can raise cortisol levels by 20 percent in a single day, which directly tells the oil glands to make more sebum. Women often see breakouts before their period because progesterone thickens the oil and makes pore linings swell.
New makeup or skincare products with thick silicones or mineral oils can create a film over pores. Certain medications like lithium, steroids, and testosterone gels list acne as one of their top three skin side effects.
Why am I getting small bumps and texture on my face instead of typical pimples?
Small bumps and rough texture often signal closed comedones, which are clogged pores that haven’t opened to the surface yet. These bumps can also be a sign of fungal acne, milia, or a condition called keratosis pilaris.
Thick moisturizers or hair products can trap dead skin cells and create these tiny bumps. If the bumps come with flushing or burning, they might actually be papulopustular rosacea rather than acne.
Dead skin cells build up more as skin ages because cell turnover slows down. This makes clogged pores more common in adults than in teenagers.
Why am I suddenly breaking out on my cheeks?
Cheek breakouts often come from things that touch the face and trap heat or bacteria[6]. Phones, dirty pillowcases, and face masks all press against cheek skin and create the perfect environment for pimples.
Cotton pillowcases can hold up to 24,000 bacteria per square inch when not washed regularly. Sweat left on the skin after exercise raises the pH level and lets acne-causing bacteria multiply three times faster.
Some people also break out on their cheeks from irritating skincare or hair products[17] that run down the sides of the face. Cheek acne in adults can also point to hormone imbalances or dietary triggers.
Why is my chin breaking out all of a sudden?
Chin and jawline breakouts are strongly linked to hormones in adults. Up to 40 percent of women with polycystic ovary syndrome first show up at the doctor with explosive jawline acne.
The chin and jaw have more androgen receptors than other parts of the face. When testosterone or other androgens rise, these areas respond by making more oil. Women often see chin breakouts in the week before their period or during perimenopause when the ratio of estrogen to testosterone drops.
Sudden severe chin acne with irregular periods may need hormone testing. A fasting panel that checks total testosterone, DHEA-S, LH, FSH, and prolactin can find PCOS or adrenal problems in 20 percent of adult women with acne.
Why is my skin breaking out even though I’m following a skincare routine?
A skincare routine might cause breakouts if the products are too harsh, too heavy, or wrong for the skin type. Products labeled non-comedogenic should score one or less on the standard pore-clogging test.
Using too many active ingredients at once can damage the skin barrier and make inflammation worse. Scrubbing hard or washing more than twice daily strips the skin and makes oil glands work overtime to compensate.
Even good routines take time to work[9]. Topical retinoids can cut inflammatory pimples by up to 60 percent, but results typically appear after 12 weeks of consistent use. Some people also break out from internal triggers like hormones or diet that skincare alone cannot fix.
What is the most effective way to stop pimples from coming back?
The most effective approach combines gentle daily habits with targeted treatments that address the root cause. Using a 2 percent salicylic acid wash twice daily can reduce early clogged pores by 28 percent after four weeks.
Prescription retinoids remain the first-line treatment because they speed up cell turnover and keep pores clear. Adding benzoyl peroxide can help kill bacteria if inflammation continues. For hormone-related acne, birth control pills or androgen blockers may be needed.
Lifestyle changes also matter. Cutting added sugar below 25 grams per day reduced acne by 50 percent in one 12-week study. Getting seven to nine hours of sleep helps control the stress hormones and insulin resistance that fuel breakouts.
Changing pillowcases every two to three nights limits bacteria transfer to the face. Wiping sweat off within 30 minutes of exercise prevents pore-clogging and bacterial growth.
Post Views: 3
References
- Why am I still breaking out? The real causes of adult acne. https://www.eurekahealth.com/resources/what-causes-acne-in-adults-en Accessed April 27, 2026
- Why Am I Breaking Out?. https://www.cedars-sinai.org/stories-and-insights/expert-advice/why-am-i-breaking-out Accessed April 27, 2026
- How Does Acne Form? 4 Steps of Inflammatory Acne Formation. https://www.acne.org/exactly-how-does-acne-form-now-that-scientists-believe-it-is-primarily-inflammatory Accessed April 27, 2026
- How to treat different types of acne. https://www.aad.org/public/diseases/acne/diy/types-breakouts Accessed April 27, 2026
- Acne: Types, Causes, Treatment & Prevention. https://my.clevelandclinic.org/health/diseases/12233-acne Accessed April 27, 2026
- Brushes should be washed once a week. https://www.verywellhealth.com/why-am-i-breaking-out-8384234 Accessed April 27, 2026
- How Hormones Affect Your Skin: A Guide for Women at Different Life Stages. https://skinandcancerinstitute.com/how-hormones-affect-your-skin/ Accessed April 27, 2026
- Signs Your Acne Is Hormonal, According to Dermatologists. https://www.schweigerderm.com/skin-care-articles/acne/signs-your-acne-is-hormonal/ Accessed April 27, 2026
- Why am I still breaking out?. https://curology.com/blog/why-am-i-still-breaking-out/ Accessed April 27, 2026
- Are these everyday foods secretly damaging your skin? Experts explain. https://www.hellomagazine.com/healthandbeauty/health-and-fitness/865022/foods-that-cause-skin-inflammation/ Accessed April 27, 2026
- Is your diet impacting your skin? Here’s what to know. https://blogs.bcm.edu/2025/02/03/is-your-diet-impacting-your-skin-heres-what-to-know/ Accessed April 27, 2026
- Are your hair care products causing breakouts?. https://www.aad.org/public/diseases/acne/causes/hair-products Accessed April 27, 2026
- Skin purging occurs when active ingredients increase cell turnover. https://www.prevention.com/beauty/skin-care/a43376866/what-is-skin-purging/ Accessed April 27, 2026
- Skin Purging or Breaking Out? 31 Things to Know. https://www.merakilane.com/skin-purging-or-breaking-out-31-things-to-know/ Accessed April 27, 2026
- 9 things to try when acne won’t clear. https://www.aad.org/public/diseases/acne/DIY/wont-clear Accessed April 27, 2026
- How To Make Your Skincare Routine More Sustainable. https://www.themodestman.com/sustainable-skincare-routine/ Accessed April 27, 2026
- Why Are You Breaking Out?. https://www.dermalogica.com/blogs/living-skin/why-are-you-breaking-out Accessed April 27, 2026