Prescription drugs and vaccines revolutionized health care, dramatically decreasing death from disease and improving quality of life across the globe. But how do researchers, universities and hospitals, and the pharmaceutical industry decide which diseases to pursue developing drugs for?
In my work as director of the Health Outcomes, Policy, and Evidence Synthesis group at the University of Connecticut School of Pharmacy, I assess the effectiveness and safety of different treatment options to help clinicians and patients make informed decisions. My colleagues and I study ways to create new drug molecules, deliver them into the body and improve their effectiveness while reducing their potential harms. Several factors determine which avenues of drug discovery that people in research and pharmaceutical companies focus on.
Table of Contents
Funding drives research decisions
Research funding amplifies the pace of scientific discovery needed to create new treatments. Historically, major supporters of research like the National Institutes of Health, pharmaceutical industry and private foundations funded studies on the most common conditions, like heart disease, diabetes and mental health disorders. A breakthrough therapy would help millions of people, and a small markup per dose would generate hefty profits.
As a consequence, research on rare diseases was not well-funded for decades because it would help fewer people and the costs of each dose had to be very high to turn a profit. Of the more than 7,000 known rare diseases, defined as fewer than 200,000 people affected in the U.S., only 34 had a therapy approved by the Food and Drug Administration before 1983.
The passage of the Orphan Drug Act changed this trend by offering tax credits, research incentives and prolonged patent lives for companies actively developing drugs for rare diseases. From 1983 to 2019, 724 drugs were approved for rare diseases.

Elise Amendola/AP Photo
Emerging social issues or opportunities can significantly affect funding available to develop drugs for certain diseases. When COVID-19 raged across the world, funding from Operation Warp Speed led to vaccine development in record time. Public awareness campaigns such as the ALS ice bucket challenge can also directly raise money for research. This viral social media campaign provided 237 scientists nearly US$90 million in research funding from 2014 to 2018, which led to the discovery of five genes connected amyotrophic lateral sclerosis, commonly called Lou Gehrig’s disease, and new clinical trials.
How science approaches drug development
To create breakthrough treatments, researchers need a basic understanding of what disease processes they need to enhance or block. This requires developing cell and animal models that can simulate human biology.
It can take many years to vet potential treatments and develop the finished drug product ready for testing in people. Once scientists identify a potential biological target for a drug, they use high-throughput screening to rapidly assess hundreds of chemical compounds that may have a desired effect on the target. They then modify the most promising compounds to enhance their effects or reduce their toxicity.
When these compounds have lackluster results in the lab, companies are likely to halt development if the estimated potential revenue from the drug is less than the estimated cost to improve the treatments. Companies can charge more money for drugs that dramatically reduce deaths or disability than for those that only reduce symptoms. And researchers are more likely to continue working on drugs that have a greater potential to help patients. In order to obtain FDA approval, companies ultimately need to show that the drug causes more benefits for patients than harms.
Sometimes, researchers know a lot about a disease, but available technology is insufficient to produce a successful drug. For a long time, scientists knew that sickle cell disease results from a defective gene that leads cells in the bone marrow to produce poorly formed red blood cells, causing severe pain and blood clots. Scientists lacked a way to fix the issue or to work around it with existing methods.
However, in the early 1990s, basic scientists discovered that bacterial cells have a mechanism to identify and edit DNA. With that model, researchers began painstaking work developing a technology called CRISPR to identify and edit genetic sequences in human DNA.
The technology finally progressed to the point where scientists were able to successfully target the problematic gene in patients with sickle cell and edit it to produce normally functioning red blood cells. In December 2023, Casgevy became the first CRISPR-based drug approved by the FDA.
Sickle cell disease made a great target for this technology because it was caused by a single genetic issue. It was also an attractive disease to focus on because it affects around 100,000 people in the U.S. and is costly to society, causing many hospitalizations and lost days of work. It also disproportionately affects Black Americans, a population that has been underrepresented in medical research.
Real-world drug development
To put all these pieces of drug development into perspective, consider the leading cause of death in the U.S.: cardiovascular disease. Even though there are several drug options available for this condition, there is an ongoing need for more effective and less toxic drugs that reduce the risk of heart attacks and strokes.
In 1989, epidemiologists found that patients with higher levels of bad, or LDL, cholesterol had more heart attacks and strokes than those with lower levels. Currently, 86 million American adults have elevated cholesterol levels that can be treated with drugs, like the popular statins Lipitor (atorvastatin) or Crestor (rosuvastatin). However, statins alone cannot get everyone to their cholesterol goals, and many patients develop unwanted symptoms limiting the dose they can receive.
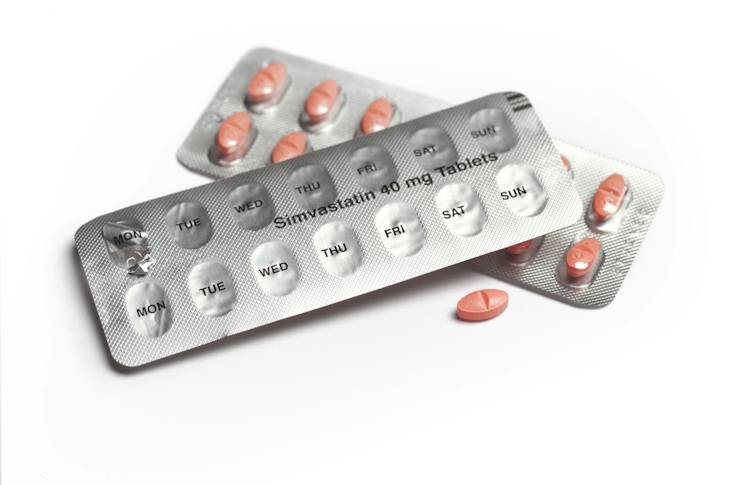
Peter Dazeley/The Image Bank via Getty Images
So scientists developed models to understand how LDL cholesterol is created in and removed from the body. They found that LDL receptors in the liver removed bad cholesterol from the blood, but a protein called PCSK9 prematurely destroys them, boosting bad cholesterol levels in the blood. This led to the development of the drugs Repathy (evolocumab) and Praluent (alirocumab) that bind to PCSK9 and stop it from working. Another drug, Leqvio (inclisiran), blocks the genetic material coding for PCSK9.
Researchers are also developing a CRISPR-based method to more effectively treat the disease.
The future of drug development
Drug development is driven by the priorities of their funders, be it governments, foundations or the pharmaceutical industry.
Based on the market, companies and researchers tend to study highly prevalent diseases with devastating societal consequences, such as Alzheimer’s disease and opioid use disorder. But the work of advocacy groups and foundations can enhance research funding for other specific diseases and conditions. Policies like the Orphan Drug Act also create successful incentives to discover treatments for rare diseases.
However, in 2021, 51% of drug discovery spending in the U.S. was directed at only 2% of the population.. How to strike a balance between providing incentives to develop miracle drug therapies for a few people at the expense of the many is a question researchers and policymakers are still grappling with.
![]()
C. Michael White does not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.