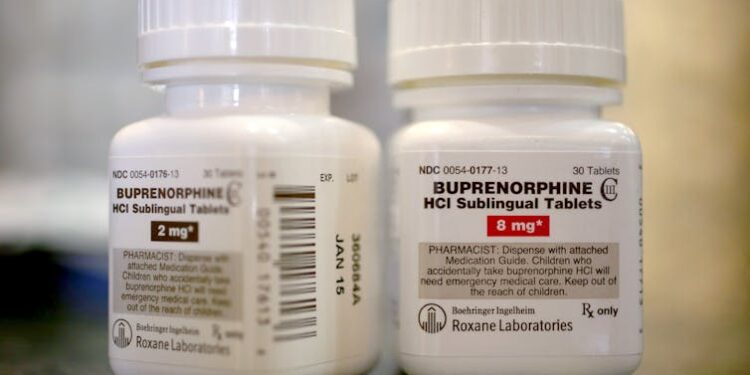
Patients who are prescribed higher daily doses of the medication buprenorphine for opioid use disorder are significantly more likely to stay in treatment. Those on 17 to 24 milligrams averaged 190 days in care compared to 90 days for those on 8 milligrams or less. Yet Black patients are less likely than white patients to receive the higher doses.
Those are the key findings of a study my colleagues and I conducted with 5,000 adults enrolled in Medicaid in Philadelphia who are prescribed buprenorphine to treat their opioid use disorder.
I am an assistant professor at University of Pennsylvania’s School of Nursing, and my research focuses on improving care and outcomes for people with opioid use disorder.
Table of Contents
Why it matters
Buprenorphine is one of the most effective treatments for opioid use disorder. Unlike most opioids, buprenorphine only partially activates opioid receptors, providing enough stimulation to prevent withdrawal and cravings while not causing euphoria. This lowers the risk of overdose.
Buprenorphine also blocks other opioids from binding to opioid receptors and causing euphoric effects. This deters patients from using other opioids while on the medication.
Across the board, patients who received higher doses of buprenorphine – usually 17 to 24 milligrams per day, but sometimes more – stayed in treatment significantly longer than those who started on medium doses of 9 to 16 milligrams, or lower doses of 8 milligrams.
Staying in treatment for opioid use disorder is important because it reduces overdose risk and provides a foundation for recovery.
Our study also revealed racial disparities.
Black patients were less likely than white patients to receive the 17 to 24 milligram prescriptions. These differences may reflect prescriber preferences, inequities in health care or misconceptions among both patients and clinicians about safe dosing.
Other groups were more likely to receive higher buprenorphine doses. Over half of our sample was diagnosed with a musculoskeletal condition – such as osteoarthritis, rheumatoid arthritis and gout – alongside opioid use disorder. These patients were more likely to receive higher doses.
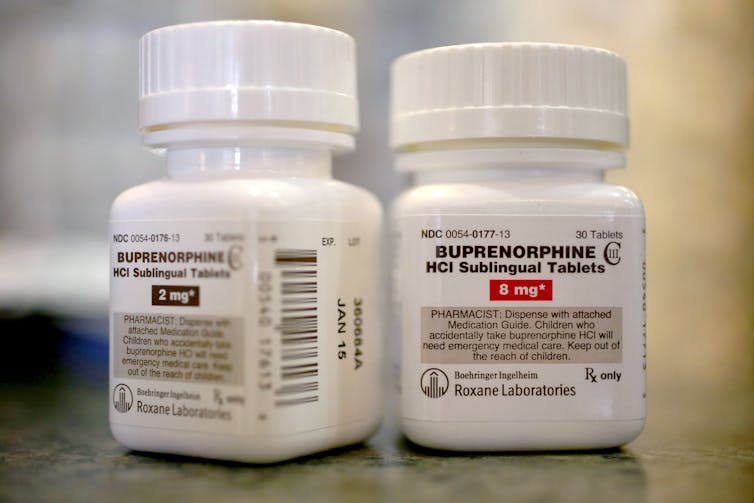
Joe Raedle/Getty Images
Why it matters
Over the past decade, the unregulated street opioid supply across the U.S. – and notably in Philadelphia – has become much more potent and unpredictable. The powerful synthetic opioid fentanyl as well as the animal tranquilizers xylazine and medetomidine are pervasive in Philadelphia. With these changes, standard buprenorphine doses may not be enough to stabilize withdrawal symptoms and prevent patients from using again.
Identifying disparities in buprenorphine dosing also sets up a number of interventions that insurers can use to address them.
For example, Community Behavioral Health, Philadelphia’s Medicaid behavioral health managed-care organization, has provided education about buprenorphine at faith‑based conferences, convened focus groups with Medicaid members to understand barriers to buprenorphine treatment, and allowed us to present our findings in a forum with local prescribers and pharmacists.
In December 2024, the U.S. Food and Drug Administration updated its recommendations about buprenorphine dosing. Previously, it supported a target dose of 16 milligrams and said that doses over 24 milligrams showed no clinical advantage.
Now, the FDA has removed the phrase “target dose” from the drug label. It also added that although doses over 24 milligrams have not been investigated in randomized clinical trials, they “may be appropriate for some patients.”
This clarification rolls back outdated language that many clinicians and insurers took to mean that 16 milligrams was the maximum for treating opioid use disorder.
What still isn’t known
Clinicians still do not fully understand patient preferences around buprenorphine dosing. Some patients may want higher doses to better manage withdrawal or cravings. Others may prefer lower doses due to concerns about not being able to discontinue buprenophrine if they are on a high dose.
The dosing patterns that we observed suggest that Black patients do not have equal access to higher doses of buprenorphine they may need. Understanding why these differences occur, and how to address them, is essential to equitable treatment.
The Research Brief is a short take on interesting academic work.
Read more of our stories about Philadelphia and Pennsylvania, or sign up for our Philadelphia newsletter on Substack.