THE CANADIAN PRESS/Chris Young
When Canada’s premiers doubled down earlier this year on their demand for a $28 billion unconditional increase in the Canada Health Transfer (CHT), they missed an opportunity to finally achieve the kind of health-care reform our underperforming system has been told it needs over and over again.
The rationale for this demand is that the system is chronically underfunded (itself a debatable contention), and this is supposedly because, as Saskatchewan Premier Scott Moe is fond of tweeting: “Ottawa used to fund 50 per cent of health care costs and now only funds 22 per cent of those costs.”
The premiers are also suggesting they’re being modest in their demands. They’re not asking for a return of the 50/50 deal struck in the 1960s, but only that Ottawa up its share to 35 per cent.
As I’ve argued previously, the premiers’ demand fundamentally misrepresents the history of health-care financing in Canada.
Read more:
The disingenuous demands of Canada’s premiers for $28 billion in health-care funding
They have forgotten that the 50/50 deal ended in 1977 with the full consent of the provincial governments. Since then, the size of the federal cash transfer for health has been subject to both intense federal-provincial diplomacy and federal unilateralism.
Their misleading take on history aside, the premiers seem determined that any increase in health funding from Ottawa pertains to the more or less unconditional general CHT, set at $45 billion to the provinces in 2022-23 — and not part of an agreement that might specify priorities for action and reform on their part.
Table of Contents
Health accords didn’t bring about change
It’s clear that national accords, like those in 2000, 2003 and 2004, did little to effect real change in the system, although the 2004 Health Accord did provide stable and predictable increases in the CHT.
When the 2004 accord expired in 2017, neither the federal nor the provincial governments were in the mood for another grand bargain. Instead, Ottawa took a very different tack. It agreed to a 3.5 per cent annual increase in the CHT (up from a three per cent from 2014 to 2017) and to provide an additional $11.5 billion in targeted funding for improvements to community and mental health care.
In order to receive the cash, provinces had to sign bilateral agreements that set out, in varying degrees of detail, where and how the money would be spent.
As a colleague and I have argued elsewhere, these bilateral agreements, though still imperfect, are a markedly improved way of increasing transparency about where health-care dollars go.

THE CANADIAN PRESS/Michael Bell
They could also serve as an accountability tool for measuring progress focused not just on fixing but actually improving Canada’s publicly administered health-care system.
In all likelihood, Ottawa will want to continue what it started in 2017 and tie any significant funding increase to a new set of bilateral agreements based on priorities chosen by the provinces. It’s just as likely that this is what the premiers are really trying to avoid.
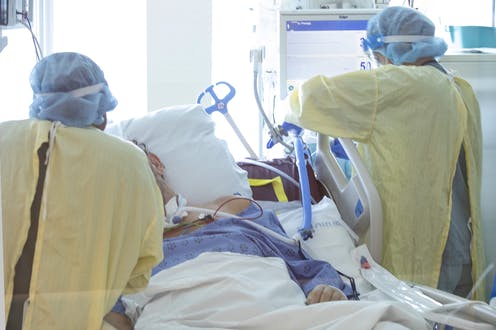
The impact of COVID-19
The COVID-19 pandemic presents us with a unique opportunity to rethink and reform public health care in Canada.
There is no doubt that the system was hit hard — its capacity was stretched, its workforce took a still uncalculated toll and all manner of service delivery was interrupted. Most notably, surgical wait times (already a serious problem in Canada’s system) were made worse, with one report indicating Ontario alone had a backlog of a million surgical procedures.
Read more:
How to solve Canada’s wait time problem
Furthermore, the pandemic exposed profound problems in long-term care and community and mental health-care systems.
It’s precisely because of so many simultaneous challenges that we should be thinking not just of rebuilding Canadian health care, but undertaking the necessary and long demanded changes that would create a 21st-century publicly funded and administered health-care system.
There are two likely scenarios.
In the first, Ottawa agrees to a significant increase in the CHT and the provinces simply take the money without making any of the necessary changes to how and what services are delivered (much as the Senate concluded happened with the $40 billion provided by the 2004 Health Accord). At best, that means we return to a pre-pandemic status quo in which the provincial systems continue to lose ground.
In the second, new agreements target the funding to remake the health-care workforce, make better progress on primary health-care reform, reconfigure long-term care, build real community-based mental health care or reconfigure the continuum of care to manage wait times on an ongoing basis.

THE CANADIAN PRESS/Graham Hughes
Co-operation from premiers needed
The second will not happen without some form of conditionality, transparency and accountability from the premiers themselves. Unfortunately, the 2017 bilateral agreements contain no obligation on the provinces’ part to report on achievements relative to their commitments.
Asking provinces to report to the federal government on how they manage their constitutional responsibilities for health care could be taken as a violation of provincial sovereignty. But they should not refuse to report to their own residents.
It’s hardly inappropriate for Ottawa to insist that provinces report to their residents on any targeted funding aimed at priorities the provinces themselves commit to tackling.
So, unless and until the premiers agree to set out — perhaps in a new set of bilateral agreements — how they intend to spend and report on the 62 per cent increase in transfers they are demanding to actually bring about real change in their respective health systems, Ottawa should refuse. And Canadians themselves should just say no.
![]()
Tom McIntosh received funding through the University of Calgary for a study of the 2017 bilateral health care accords.
























