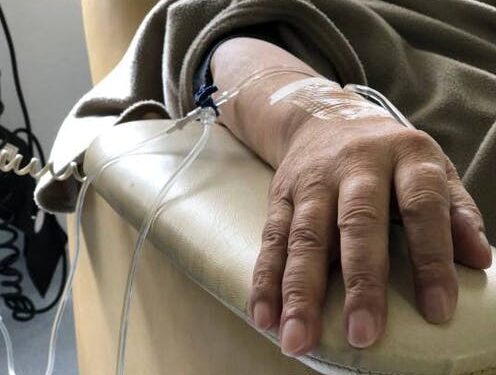
Rarely does an oncologist closely question a breast cancer patient about their blood glucose, body weight, lipid profile, or medications for diabetes and cardiovascular disease. Instead, these issues are usually the concern of the patient’s primary care provider.
Medical experts have recognized that obesity, defined as a body mass index of 30 or greater, increases the risk of several cancers. They include cancers of the breast, esophagus, kidney, gallbladder, liver, colon and several other organs. We have been aware of this relationship for about 20 years. Despite this awareness, medicine is still missing a holistic view of people with cancer.
When testing new cancer drugs, clinical trials traditionally exclude patients with a history of heart disease, kidney disease, diabetes or similar chronic conditions related to obesity. The purpose is to make study results easier to interpret. But this practice leaves cancer researchers with a weak understanding of how patients could be monitored and treated for obesity-driven cancers. One way it limits their knowledge is by leaving out significant numbers of patients. Among them are patients of color, who are already underrepresented in scientific studies generally and cancer treatment treatment trials in particular.
As a molecular oncologist at Boston Medical Center, I explore how metabolic conditions like obesity and diabetes can influence whether someone develops cancer. I look closely at how these conditions can affect how the cancer grows, spreads or responds to treatment.

Juan Ruiz Parmo/iStock via Getty Images Plus
Our teams at Boston Medical Center’s Cancer Center have have identified how obesity and diabetes may provoke cancer to spread in potentially deadly ways. In particular, insulin-resistant fat cells are likely to play a critical role in provoking breast cancer cells to move from the original tumor to distant organs like the lungs, liver, bones or brain. These distant metastases commonly define the end stage before someone with breast cancer dies.
Our results show that in the microscopic neighborhood inside or near a tumor, cancer cells and noncancerous fat cells sit right next to each other, like neighbors on a park bench. Our research has shown that these two cell types engage in active “cross-talk.” This communication may inhibit or promote a tumor’s ability to grow and spread. How that happens is not well understood, partly because oncologists – whether studying cancer or treating it – generally don’t take nearby fat cells into consideration.
Strategic diagnosis and treatment
Acknowledging the relationship between fat cells and cancer cells offers opportunities to find and treat cancer less invasively. With molecules isolated from just a teaspoon or less of a patient’s blood, specialists can learn the risk that the cancer might be growing and spreading. These molecules, called biomarkers, can also show which patients are in the greatest danger of treatment failure. Taking occasional blood samples is less invasive than repeated biopsies, which involves getting samples of breast or other tissue.
When endocrinologists and oncologists consult with one another, they can consider obesity and metabolism alongside the current standard of care for patients with cancer. This combination would likely benefit populations, like older adults, in which both obesity and metabolic disease are more prevalent.
Furthermore, the cancer patient population may soon include more young people. A 2019 study found that people age 50 or younger have a disproportionately elevated risk for certain obesity-driven cancers, including obesity-associated colorectal cancer. The relationship between fat cells and cancer cells could explain some of these trends.
Closing gaps in care
And already, more young African American adults are developing aggressive colorectal cancers than young adults of other races. This fact came to the nation’s attention in 2020, when actor Chadwick Boseman died from an aggressive colon cancer at age 43.
Although Boseman was not overweight, his death brought attention to the community of African American adults who experience higher risks not only for obesity and diabetes but also for several cancers including prostate, breast and colorectal. And despite their higher risks, Black patients are often not effectively counseled by physicians regarding cancer risk and treatment.
[Get fascinating science, health and technology news. Sign up for The Conversation’s weekly science newsletter.]
At Boston Medical Center, 50% of our patients have diagnoses of obesity and 30% have Type 2 diabetes. We see similar numbers and patterns in our cancer patient population. One potential reason is that Boston Medical Center is a safety-net hospital, providing essential and excellent care to a very diverse range of patients regardless of insurance, immigration status or medical literacy. Such hospitals are often located in neighborhoods with high rates of obesity and diabetes.
Black and Latino adults with cancer tend to be overrepresented in safety-net hospital systems. They receive cancer screenings less often. They also experience
longer wait times, first for diagnosis and then for treatment. These factors contribute to worse survival rates among Black and Latino cancer patients. Some of these worse outcomes may be a result of cancer and diabetes interacting in these patients.
Addressing disparities like these would be a natural benefit of bringing together previously disconnected clinical specialties. Research on the linkage among obesity, diabetes and cancer is revealing new pathways and molecules that tie these different diseases together. These new insights could improve outcomes for patients who are at greatest risk, and prompt more holistic assessments and treatments for all patients.
![]()
Gerald Denis receives funding from the National Cancer Institute.